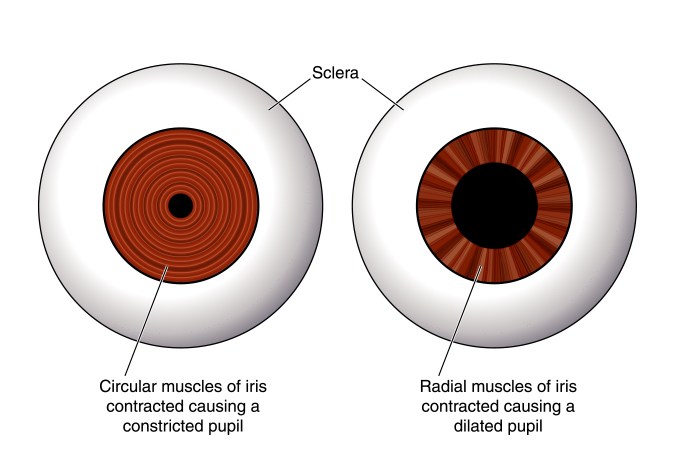
Although these tests are generally tried and true, one is best left alone with a preference for the first two. Three major methods exist to determine the presence of an APD (Table 1). Subjective and requires technical skill for subtle APDs.APD recorded in healthy subjects at times.Long test duration and lack of test standardization.Comparison of Pupil Testing Methods and Their Application 6 Therefore, practitioners’ ability to determine the presence of an APD is a critical step in caring for patients suffering from glaucoma as well as those suffering from other types of optic neuropathies. It is well documented that patients with glaucoma exhibit lower amplitude, slower velocity and acceleration of pupil subjects when compared with healthy controls. Though glaucoma is typically a bilateral condition, it often initially presents unilaterally or bilaterally with variation in severity between the two eyes. 5 APD and Glaucomaĭetermining the presence or absence of an APD is of great clinical value, particularly in guiding the practitioner in the course of treatment for their glaucoma patients. The efferent arm consists of the nerve impulse that exits the midbrain, traveling along the oculomotor nerve to the ciliary ganglion, resulting in constriction of both pupils in a healthy patient. The pupil response to light is best explained through the understanding of the light reflex pathway, which is comprised of two arms: the afferent and the efferent.Īs the first arm, the afferent portion signifies the nerve impulse sent from stimulation of the retinal ganglion cells (RGCs) to the optic nerve by light, continuing down the optic tract, decussating at the chiasm and ultimately reaching the pretectal nucleus of the midbrain. Unilateral glaucoma, as seen in these fundus photos, more severe in the right eye than the left, could elicit an APD in the right eye. Understanding both, however, will provide a fuller picture of your patient’s pathology. 3īecause it’s so commonplace, clinicians may tend to focus more on its diagnostic role than the physiology being tested. 1-4 It serves as an indication of reduced afferent input from the retina or optic nerve when compared with the fellow eye. 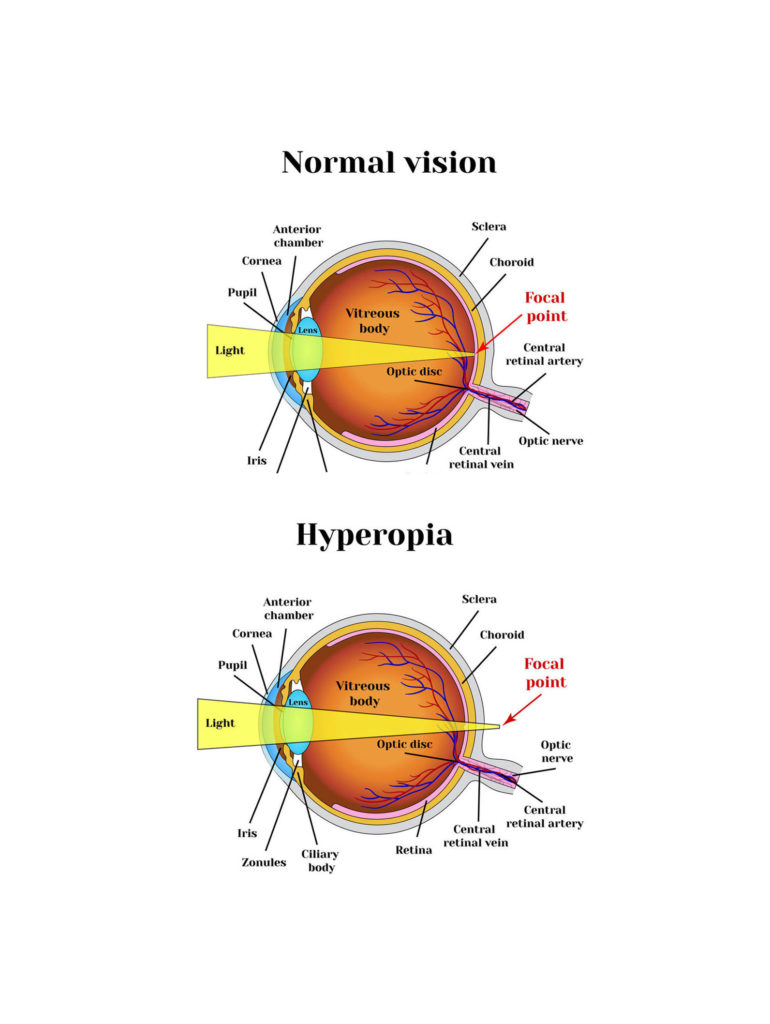
1 A relative afferent pupillary defect (APD), when present, is an important marker in the evaluation of unilateral or asymmetric function of the anterior visual pathway. The testing of the pupillary response to light is routinely performed by the eye care practitioner and imparts valuable information regarding the presence, laterality or magnitude of diseases that mainly affect the optic nerve, such as glaucoma.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
